
Corneal transplantation, vision restoration and life change
5min ReadCorneal transplantation, also known as keratoplasty, is a significant surgical procedure that involves replacing a damaged cornea with a healthy cornea from a deceased donor. This life-changing procedure has the power to restore vision, reduce pain, and significantly improve the quality of life for people with various corneal conditions.
Recognition of the Cornea
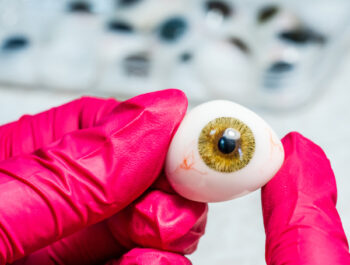
Before diving into the intricacies of corneal transplantation, it is important to understand the importance of the cornea itself. The cornea is the outermost transparent and dome-shaped layer of the eye that covers the iris and pupil. It plays a vital role in focusing incoming light on the retina and enabling clear vision. However, due to diseases, infections, injuries or genetic disorders, the cornea can be damaged, resulting in impaired vision or even complete blindness.
Method
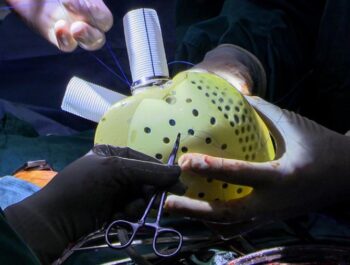
Corneal transplant surgery involves removing the damaged or cloudy cornea and replacing it with a healthy donor cornea. There are several types of corneal transplant techniques, including penetrating keratoplasty (PK), deep anterior lamina keratoplasty (DALK), and endothelial keratoplasty (EK).
Impaired keratoplasty (PK):
PK is the traditional method used for corneal transplantation. It involves replacing the full thickness of the cornea using a circular blade or laser to create a central button-shaped graft. This procedure is usually performed when the disease involves the entire cornea, including all its layers.
Deep anterior laminar keratoplasty (DALK):
DALK is a partial-thickness corneal transplant technique that involves removing only the diseased or scar tissue, leaving the patient’s healthy innermost layer of the cornea (the endothelium) intact. This method is preferred in cases where the disease is limited to the outer layers of the cornea, such as certain types of corneal dystrophy.
Endotlial kratoplasty (EK):
EK procedures involve replacing only the innermost layer of the cornea, known as the endothelium. This technique is used when the dysfunction is only related to endothelial cells, which are responsible for maintaining corneal transparency and reducing corneal edema. EK includes Descemet’s Stripping Endothelial Keratoplasty (DSAEK) and Descemet’s Membrane Endothelial Keratoplasty (DMEK), which differ in the thickness of the graft used.
Corneal graft rejection
Corneal transplants are being performed regularly and have an acceptable success rate. In fact, the cornea has the best tissue transplant results. If corneal graft rejection is detected quickly, it can be prevented in 9 out of 10 cases.
Like any other surgical procedure, corneal transplantation is associated with certain risks. But for most people, the improved vision loss outweighs the potential complications associated with corneal transplant surgery. Corneal transplant complications are significant and can include graft rejection, eye infections, and problems with suture use.
Rejection of donor tissue after a cornea transplant is the most serious complication and occurs in 5 to 30 percent of patients. Transplant rejection means that your immune system recognizes the transplant as a disease and destroys it. Research shows that having glaucoma and corneal swelling associated with cataract surgery can increase the chance of transplant rejection.
Identifying the main warning signs after transplant is the first step to prevent transplant failure. These can be remembered using RSVP:
- Eye redness
- Extreme sensitivity to light
- Reduced vision
- Pain
Transplant rejection symptoms may appear one month or several years after surgery. The doctor will prescribe drugs that can reverse the rejection process. According to the American Cornea Research Foundation, if this condition is detected early, the transplant will be successful in 9 out of 10 cases.
If your transplant fails, the transplant surgery can be repeated.
Advances in corneal transplantation:
In recent years, corneal transplant techniques have seen significant improvements, leading to improved outcomes and improved vision for patients. One of these advances is the use of femtosecond laser technology, which has revolutionized corneal transplant surgeries by creating precise incisions and better wound healing. In addition, selective suturing techniques and the development of new tools have refined surgical procedures, leading to reduced complications and faster recovery times.
Corneal transplantation has revolutionized lives around the world, offering hope to those who have lost their vision due to corneal disease or injury. By restoring clarity to the cornea, patients can regain functional vision, often eliminating the need for opacified glasses or contact lenses. The impact of corneal transplantation goes beyond the physical aspect. It restores independence, increases self-esteem and enables people to participate fully in their personal and professional lives.
Challenges:
While corneal transplantation has been very successful, there are challenges that must be addressed. A major challenge is the shortage of donor corneas, as demand far exceeds supply. Global efforts to increase awareness of organ donation and facilitate the efficient recovery and distribution of corneas are critical in bridging this gap.
In addition, ongoing research aims to improve the longevity of transplanted corneas by developing innovative techniques for tissue preservation, reducing graft rejection rates, and exploring alternative sources of corneal tissue such as synthetic materials or laboratory-grown corneas using stem cells.
As a result, corneal transplant surgery has emerged as an extraordinary medical procedure that restores vision, alleviates suffering, and transforms lives. With advances in surgical techniques and ongoing research, the future promises to further improve outcomes and increase access to corneal transplantation. As we continue to push the boundaries of medical science, corneal transplants touch the lives of countless people and empower them with the precious gift of sight.









Reviews
Number of pending reviews175