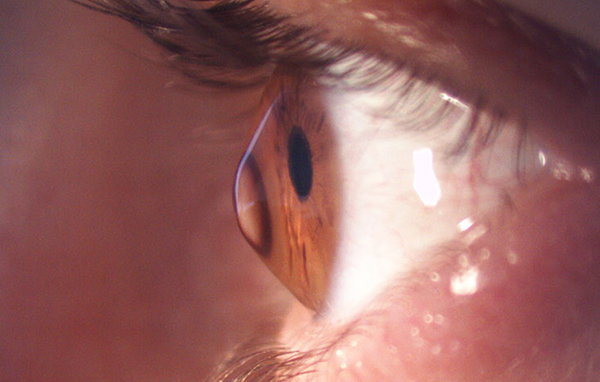
What is keratoconus ?
3min ReadKeratoconus is a disease and a non-inflammatory phenomenon of the eye, in which the eye changes from spherical and thin to a conical state, and the natural shape of the eye is lost, causing reduced vision and astigmatism. This disease starts in youth and puberty and continues until the age of 35, 40 years. The earlier this disease is detected, the easier it is to treat and prevent the progress of this disease. Corneal keratoconus causes blurring and weakening of the eyes and disturbs a person’s vision. While the exact cause of keratoconus is still unknown, several factors may play a role in its development, including genetic predisposition, abnormalities in collagen production, chronic eye rubbing, and some eye diseases.
Symptoms:
Symptoms of keratoconus can vary from mild to severe and may include the following:
- Blurred or distorted vision
- Frequent changes in glasses
- Increased sensitivity to light and glare
- Difficulty driving at night
- Burning and eye itch
- Eye fatigue and headache
Diagnosis:
An ophthalmologist can diagnose keratoconus through a comprehensive eye exam, including a detailed medical history, vision tests, corneal imaging, and corneal thickness measurements. Specialized imaging techniques such as corneal topography and optical coherence tomography (OCT) may also be used to assess the shape and thickness of the cornea.
Complications due to keratoconus :
Depending on the patient’s condition, the rate of progression of keratoconus can be different. There are cases in which the cornea swells at a high speed, followed by a corneal ulcer and a severe decrease in vision. The appearance of these symptoms is caused by the rupture of one of the important inner layers of the cornea and the entry of fluids into the cornea. In such cases, the swelling and inflammation created in the cornea will disappear by itself, and the most important side effects will be a severe decrease in vision.
Treatment options:
A)Glasses and contact lenses: In the early stages of keratoconus, glasses or soft contact lenses may be sufficient to correct vision. However, as the disease progresses, specialized contact lenses such as rigid gas permeable (RGP) or scleral lenses may be recommended. These lenses are placed over the distorted cornea, providing clearer vision and improving comfort.
B)Corneal cross-linking (CXL): Corneal cross-linking is a minimally invasive procedure that aims to strengthen the cornea and stop the progression of keratoconus. It is the cornea. During this procedure, the eye is exposed to ultraviolet light and riboflavin (vitamin B2), which causes the formation of new collagen fibers and strengthens the structural integrity of the cornea.
C)Intrastromal corneal rings (ICR): ICRs, also known as corneal implants or intakes, are small, semicircular plastic devices that are inserted into the cornea to reshape the curvature of the cornea. By correcting the shape of the cornea, ICRs can improve vision and reduce astigmatism, thereby increasing the quality of vision.
- D) Corneal transplant: In severe cases of keratoconus where other treatments are not effective, corneal transplant may be considered. This procedure involves replacing the damaged cornea with a healthy donor cornea. However, corneal transplantation is usually reserved for advanced cases of keratoconus due to the risks and recovery time involved.
Corneal hump and LASIK
In LASIK and other laser surgeries (such as PRK, LASIK, etc…), a change in shape of the cornea is created with the use of a laser, and a part of the cornea is cut and separated. Therefore, after the LASIK operation, we expect the cornea to be thinner than its original state. As mentioned, keratoconus is a progressive disease that leads to thinning of the cornea, so the combination of unpredictable changes resulting from keratoconus and LASIK can lead to irreparable damage to the cornea. For this reason, LASIK is not recommended for people with keratoconus.
Conclusion:
keratoconus is a progressive eye disease that requires early diagnosis and appropriate treatment to prevent further deterioration and maintain visual function. With the advancement of technology and various treatment options available, people with keratoconus can improve their vision and improve their quality of life. If you experience symptoms or suspect keratoconus, it is important to consult an eye care professional for a complete evaluation and personalized treatment plan.










Reviews
Number of pending reviews174